key takeaway
Despite being eligible, many Californians lose vital Medi-Cal coverage due to complex paperwork and difficulty reaching county offices. Streamlining the renewal process and improving accessibility are crucial to ensure everyone keeps the health insurance they need.
Continuous access to health care is necessary for everyone to be healthy and thrive. Unfortunately, paperwork challenges often prevent people from obtaining and maintaining health coverage. A clear example of this: Too many individuals continue to be disenrolled from Medi-Cal, California’s Medicaid program, due to paperwork challenges.
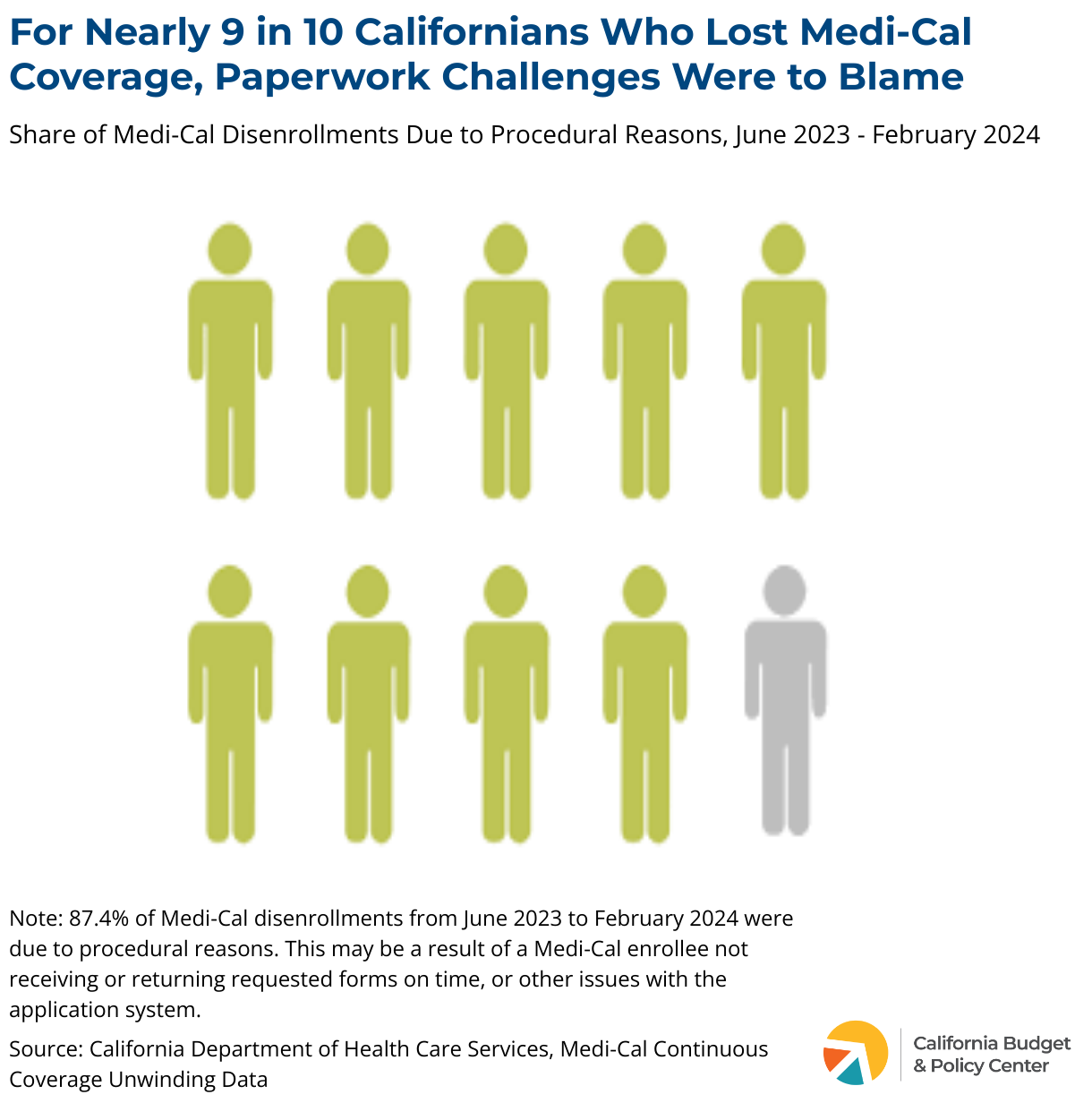
Last year, California began processing Medi-Cal renewals for the first time since the start of the pandemic. As a result, over 1.4 million Californians have lost Medi-Cal coverage from June 2023 to February 2024. About 9 in 10 Californians (87.4%) who lost Medi-Cal coverage during this period did so because they did not complete the renewal paperwork or had incorrect or missing information in their forms.
Completing the renewal process often involves complex paperwork and documentation requirements, which can be difficult to navigate. Additionally, many Californians have experienced extended call wait times when attempting to contact county Medi-Cal workers regarding their application.
Certain groups, including older adults and people with disabilities, are at greater risk of losing Medi-Cal coverage during the unwinding period.1Jennifer Tolbert and Meghana Ammula, 10 Things to Know About the Unwinding of the Medicaid Continuous Enrollment Provision (Kaiser Family Foundation, June 2023). Immigrants and their family members face unique obstacles in remaining covered, such as language barriers, privacy concerns, and fear of immigration-related consequences. Many Californians who are losing Medi-Cal coverage due to paperwork challenges may still meet the eligibility criteria.2Of the redeterminations that were received and processed in February 2024, about 9% were ineligible. See California Department of Health Care Services, Medi-Cal Continuous Coverage Unwinding Dashboard (February 2024), 14.
The high disenrollment rate due to paperwork challenges underscores the need to further streamline the renewal process and alleviate the paperwork burden on beneficiaries during the unwinding period and beyond. Addressing these challenges is essential to ensure that those who are eligible for Medi-Cal continue to receive vital health coverage.
While state leaders have implemented measures to reduce barriers to accessing and maintaining Medi-Cal coverage, they can take additional steps to prevent Californians who remain eligible for Medi-Cal from losing coverage. These include:
- Permanently extend unwinding flexibilities.
- Improving wait times for county call centers.
- Accelerating the implementation of continuous Medi-Cal coverage for children from birth to age 5.
- Providing continuous Medi-Cal coverage to adults.
- Increasing reimbursement rates for Community Health Workers / Promotoras/ Representatives (CHWPRs).
By taking additional action, state leaders can reduce barriers and ensure that all Californians, regardless of race, age, disability, or immigration status, can access and maintain the critical health coverage they need to be healthy and thrive.